What is the HIPAA Privacy Rule?
The HIPAA Privacy Rule is crucial for protecting PHI and ensuring patient privacy. Learn about HIPAA PHI compliance with our free guide.

The HIPAA Privacy Rule is crucial for protecting PHI and ensuring patient privacy. Learn about HIPAA PHI compliance with our free guide.

The Privacy Rule is an important part of HIPAA that helps healthcare organizations protect data. Before we explain the Privacy Rule and how to follow it, here is some background on HIPAA:
HIPAA is a federal law. It was created to:
See also: HIPAA FAQs
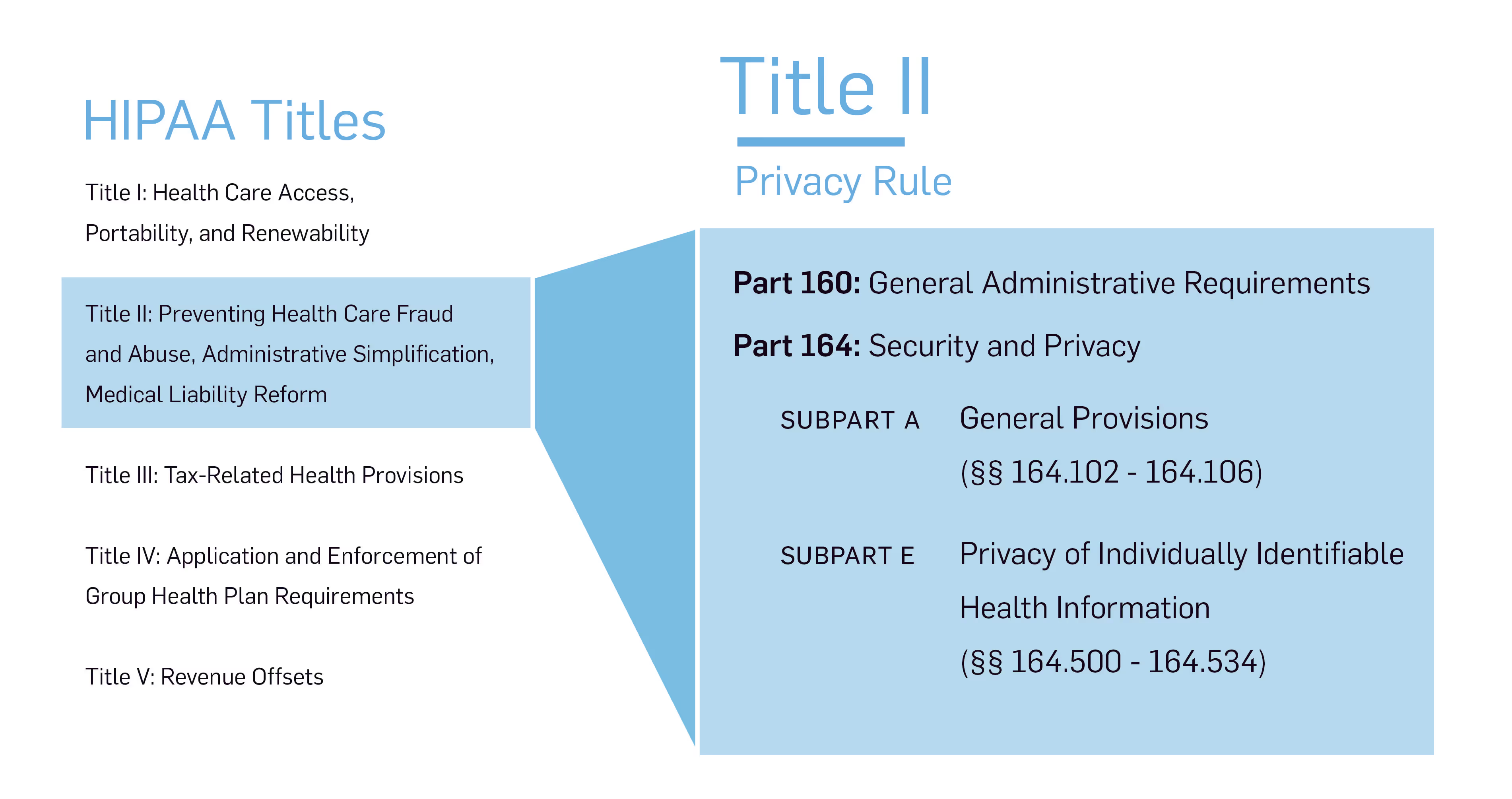
HIPAA is an acronym for the Health Insurance Portability and Accountability Act of 1996 (Public Law 104-191). It has five parts, or titles. These go along with the above-mentioned purposes of HIPAA:
The Privacy Rule establishes standards to protect an individual’s medical records and other protected health information (PHI). It concerns the uses and disclosures of PHI and defines an individual’s rights to access, and regulates how their medical information is used.
The HIPAA Privacy Rule is described in the following locations in the CFR:
The Privacy Rule strives to assure that an individual’s health information is properly protected. At the same time, it allows access to the information needed to ensure high-quality health care for patients and to protect the public. The Privacy Rule strikes a balance that permits important usage of information, while protecting the privacy of people who require health care services.
When it comes to the HIPAA Privacy Rule, healthcare organizations might think they have everything covered. You likely have your privacy practices posted throughout your workplace and believe that instances where employees leak PHI to the public are rare.
However, finding where PHI exists in an organization can be a complex effort, especially when that information is digital. Making sure PHI is secured from improper disclosure often requires expert help. For example, it’s not uncommon for healthcare providers to leave out the following in their policies, procedures, or risk analyses:
If covered entities or their employees do intentionally obtain or disclose PHI in violation of the HIPAA Privacy Rule, penalties are serious. Organizations can be assessed civil monetary penalties up to $50,000 per violation with a penalty cap of $1.5 million for multiple violations of an identical requirement in a calendar year.
Criminal penalties are also possible. A person who knowingly obtains or discloses PHI may face a criminal penalty of up to $50,000 and up to one-year imprisonment. These increase to $100,000 and up to five years imprisonment if PHI is obtained or disclosed in circumstances involving false pretenses, and they increase to $250,000 and up to 10 years imprisonment if the wrongful conduct involves the intent to sell, transfer, or use identifiable health information for commercial advantage, personal gain, or malicious harm. The Department of Justice is responsible for criminal prosecutions under the Privacy Rule.
First, make sure you have policies and procedures established that clearly describe how you share PHI. And you are required to disclose PHI under some circumstances, for instance:
You’re allowed (but not required) to use and disclose PHI without an individual’s authorization under the following situations:
There are some exceptions to these rules. For example, disclosures of psychotherapy notes require written authorization from patients. Also, you typically must receive patient authorization to use and disclose PHI for marketing purposes, unless it fits within HIPAA exceptions.
Understand “Minimum Necessary.” The Minimum Necessary requirement is a core principle of the Privacy Rule. It states that only those who need to see PHI to do their jobs should get to see it, and unless you have a specific need for the information, access must be restricted. For example, a receptionist probably doesn’t need to see the X-rays of a patient to do their job.
Limit access to PHI. This should be accomplished through a combination of policies (describing intent), procedures (outlining how access should take place), and tools that restrict access to electronic PHI.